How to create a medical image management strategy

Advanced imaging technologies generate large volumes of complex data. Computed Tomography (CT), Magnetic Resonance Imaging (MRI), Ultrasound, and various specialized modalities are essential for diagnostics, treatment planning, and ongoing patient management.
Yet, the sheer quantity of images—acquired through different systems and formats—can overwhelm healthcare organizations if not properly managed.
An effective medical image management strategy ensures patients receive timely, accurate diagnoses and treatments. Beyond patient outcomes, robust image management safeguards data security, maintains regulatory compliance, and streamlines clinical workflows.
Establishing a cohesive approach to handling imaging data is no longer optional—it is a strategic imperative that directly influences an organization’s financial performance and reputation.

Why Medical Image Management Matters
Data Overload and Complexity
Medical imaging technologies continue to evolve, producing higher-resolution images and more advanced diagnostic data. While such innovation is invaluable for patient care, it results in exponential data growth. Managing this influx of large imaging files can strain network infrastructures and slow retrieval times, hampering clinical decision-making.
Ensuring Patient Safety and Outcomes
Delays or errors in image retrieval and interpretation can significantly impact patient safety. Missing or inconsistent imaging data may result in misdiagnoses, redundant imaging studies, or delayed treatments. A structured image management system addresses these risks, ensuring the right data is available at the right time.
Compliance and Data Security
Healthcare organizations face stringent regulatory requirements—like HIPAA in the U.S. and GDPR in the EU—that govern patient data handling, storage, and sharing. Non-compliance can lead to hefty fines, reputational damage, and legal liabilities. A robust image management strategy enforces secure data storage, controlled access, and comprehensive audit trails, all critical for compliance.
Operational and Financial Efficiency
Inefficiencies in managing imaging data—such as underutilized equipment or fragmented workflows—can inflate operational costs and reduce overall productivity. Organizations can lower expenditures, enhance staff efficiency, and ultimately deliver better patient services by centralizing and streamlining imaging workflows.
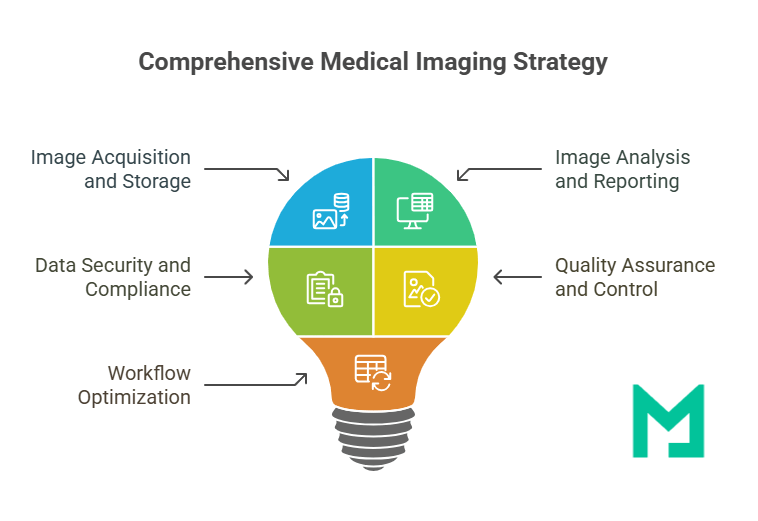
Key Components of an Effective Medical Image Management Strategy
A compelling image management strategy is a multi-layered framework that addresses technology, people, and processes. Below are the main components you should consider:
- Image Acquisition and Storage
- PACS (Picture Archiving and Communication System): The heart of most imaging strategies. A robust PACS solution centralizes images from various modalities, making them easily accessible for clinicians.
- VNA (Vendor Neutral Archive): A VNA can store images in a non-proprietary format, ensuring compatibility across different systems and vendors.
- Image Analysis and Reporting
- AI and Machine Learning (ML): Advanced algorithms help analyze images more efficiently, flag potential anomalies, and reduce human error.
- Automated Reporting: Integration with existing EMRs/EHRs enables radiologists and clinicians to quickly generate and store detailed reports, improving turnaround times.
- Data Security and Compliance
- Secure Storage and Encryption: Encryption at rest and in transit is crucial to meet privacy standards.
- Access Controls: Role-based permissions ensure only authorized personnel can view or modify sensitive data.
- Audit Trails: Comprehensive logging allows for monitoring all access and usage patterns, which is essential for regulatory audits.
- Quality Assurance and Control
- Regular Calibration: Imaging equipment must be maintained and calibrated periodically to ensure consistent image quality.
- Standardized Protocols: Using standardized imaging protocols (e.g., from the American College of Radiology) helps maintain uniform quality levels.
- Workflow Optimization
- Automated Workflows: Automated task routing and alerts ensure that images and reports get to the right people promptly.
- Cross-Department Collaboration: Collaboration tools reduce communication bottlenecks and prevent siloed information.
These components must be integrated into an overarching system for scalability, data interoperability, and continuous improvement. Addressing these fundamentals builds a robust foundation for better clinical outcomes and operational performance.
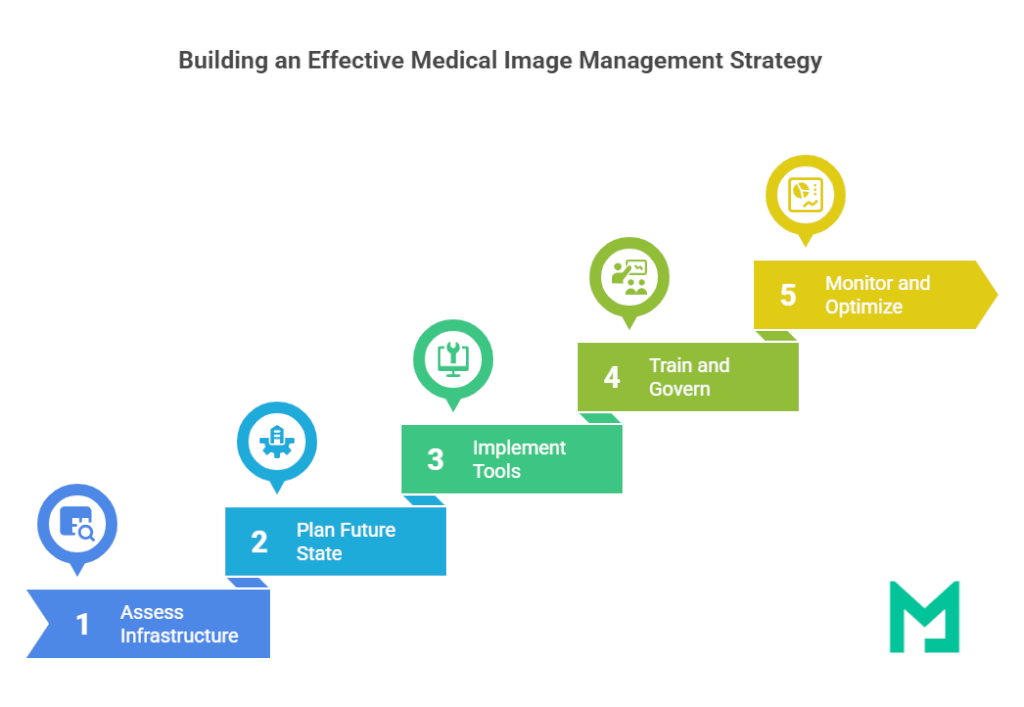
Step-by-Step Guide to Creating a Medical Image Management Strategy
Below is a structured framework to help you systematically develop and implement a medical image management strategy:
- Assess Current Infrastructure and Requirements
- Inventory Existing Systems: Document current imaging modalities, PACS, data storage solutions, and network capabilities.
- Identify Gaps: Determine shortcomings in bandwidth, interoperability, and data security.
- Define Organizational Objectives: Align imaging goals (e.g., faster turnaround, reduced costs, compliance) with broader institutional targets.
- Plan the Future State
- Technology Selection: Decide whether to upgrade or replace your PACS and whether a VNA is needed for improved data sharing.
- Integration Strategy: Map out how new systems will integrate with current EMRs, data warehouses, or analytics platforms.
- Budgeting and Timeline: Estimate costs for hardware, software licenses, implementation, and training. Set realistic milestones for rollout.
- Implement Tools and Protocols
- Systems Deployment: Install, configure, and test the selected PACS/VNA solutions.
- Security and Compliance: Implement encryption, role-based access, and compliance checklists (HIPAA, GDPR, etc.).
- Standardize Imaging Protocols: Collaborate with radiologists and technicians to ensure uniform protocols across modalities.
- Train and Govern
- Staff Training: Provide hands-on sessions for radiologists, clinicians, and IT staff. Ensure they know how to use new software tools, retrieve images, and follow compliance measures.
- Governance Model: Establish a cross-functional committee (IT, Radiology, Compliance) that sets policies, monitors performance, and enforces best practices.
- Continuous Monitoring and Optimization
- Performance Metrics: Track turnaround times, data accuracy, and equipment utilization.
- Feedback Loops: Encourage staff to report inefficiencies, system lags, and potential areas of improvement.
- Iterate and Update: Regularly update systems, train staff on new features, and refine workflows based on collected data.
Common Challenges and Solutions
Even the most carefully planned strategies can encounter obstacles. Below are frequent challenges and proposed solutions:
- Interoperability Issues
- Challenge: Many imaging systems use proprietary formats, making data sharing across disparate platforms difficult.
- Solution: Adopt VNAs to standardize image storage formats and enable seamless data exchange among various departments and locations.
- Bandwidth and Infrastructure Limitations
- Challenge: High-resolution imaging files require significant storage and network capacity, sometimes overwhelming existing IT infrastructure.
- Solution: Invest in scalable storage solutions (on-premises, cloud, or hybrid) and upgrade network bandwidth. Implement efficient compression algorithms for faster image transmission without sacrificing quality.
- Staff Resistance or Limited Training
- Challenge: Radiologists, technicians, and other clinicians may resist adapting to new systems, tools, or workflows.
- Solution: Conduct regular, role-based training sessions and provide ongoing support. Highlight time-saving features and how these tools improve patient care to encourage adoption.
- Regulatory Compliance and Legal Risks
- Challenge: Non-compliance can lead to heavy fines and reputational damage. Managing patient privacy across multiple systems intensifies legal risks.
- Solution: Establish clear data handling policies, enforce stringent access controls, and use encryption. Conduct routine audits and maintain thorough documentation to demonstrate compliance.
By proactively addressing these challenges, healthcare organizations can avoid pitfalls, minimize disruptions, and realize the full potential of their imaging strategy.
Example Scenario: A Mid-Size Hospital Implementation
Consider a mid-size hospital with multiple diagnostic imaging modalities—CT, MRI, and Mammography—spread across several departments. Each department has historically managed its storage and retrieval system, leading to fragmented data, occasional duplicate imaging, and inconsistent reporting formats.
- Infrastructure Assessment: The hospital’s leadership discovers outdated PACS software, insufficient storage capacity, and a need for better interoperability with the existing EMR.
- Strategic Planning: They decide to implement a new PACS combined with a VNA to unify image storage.
- Deployment: The IT team installs and tests the solution over six months, migrating historical images to the new system.
- Training and Governance: Radiology staff and clinicians receive training on the new workflows. A governance committee regularly reviews system usage and performance metrics.
- Outcome: The hospital reduces duplicate imaging by 25%, halves image retrieval times, and improves patient satisfaction and compliance readiness.
Conclusion and Next Steps
A medical image management strategy is a cornerstone for modern healthcare organizations aiming to deliver efficient, high-quality patient care.
Integrating a robust PACS or VNA, employing AI-driven analysis, enforcing strict security protocols, and optimizing clinical workflows establishes a reliable imaging ecosystem that benefits patients, clinicians, and administrative staff. Equally important is continuous performance monitoring and adherence to compliance standards to maintain a scalable, future-ready solution.
If you are in the planning phase, start by thoroughly assessing your current infrastructure and identifying critical gaps in technology, compliance, or workflow efficiency. In each process step, engage stakeholders—from radiologists and IT directors to compliance officers—to ensure alignment with organizational goals.

Related Articles


Lets get in touch!
Learn more about how Medicai can help you strengthen your practice and improve your patients’ experience. Ready to start your Journey?
Book A Free Demo
