The role of imaging for patient selection for thrombectomy
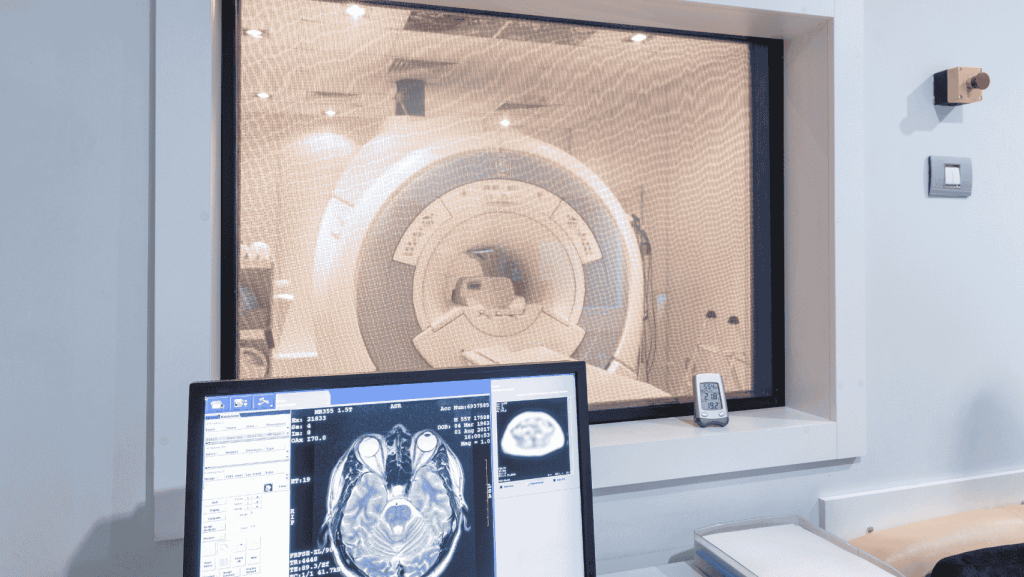
Imaging plays a critical role in patient selection for thrombectomy, a procedure used to remove a blood clot from a blood vessel.
When a big cerebral vessel is blocked, thrombectomy is a very successful treatment for a severe ischemic stroke. The prompt and accurate selection of eligible patients is necessary for the operation to be successful. Identification of patients who would benefit from thrombectomy and the location, size, and extent of the blood clot depend heavily on imaging techniques, such as computed tomography (CT) and magnetic resonance imaging (MRI).
Computer tomography
The initial imaging technique used to assess individuals with suspected stroke is computed tomography (CT). The presence of cerebral hemorrhage, which is a contraindication to thrombectomy, can be immediately and precisely detected by CT scans. The location and severity of ischemia injury, which is crucial for patient selection, can also be determined by CT scans. The amount of the ischemic penumbra, the region of the brain that is at risk of degeneration but may still be saved with prompt treatment, can be assessed using CT perfusion scans, which are particularly effective at measuring blood flow in the brain. This information is essential for figuring out whether patients qualify for thrombectomy and for directing medical decisions.
Magnetic Resonance Imaging
Magnetic Resonance Imaging (MRI) is another important imaging modality used for patient selection for thrombectomy. Compared to CT, MRI offers a more accurate picture of the brain and can be used to determine the underlying causes of a stroke, such as big vessel blockage, small vessel illness, or cardioembolic origins. The vitality of brain tissue can be determined by MRI, which is helpful for assessing the patient’s prognosis and the possible benefits of thrombectomy. Diffusion-weighted imaging (DWI) and perfusion-weighted imaging (PWI), in particular, can offer comprehensive details regarding the severity of the ischemia injury and the possibility of effective revascularization.
Angiography
Angiography is a diagnostic test that provides a visual representation of the blood vessels in the brain.
Angiography can be performed using either traditional catheter-based techniques or newer, minimally invasive techniques such as CT angiography or MRI angiography. The results of an angiography can be used to choose the best patients for thrombectomy by determining the extent and location of the blood clot. In some circumstances, angiography may also be utilized to direct the actual thrombectomy procedure, assisting the interventional neuroradiologist in locating and removing the blood clot.
Transcranial Doppler
Transcranial Doppler (TCD) is a non-invasive ultrasound technique that can measure blood flow in the brain. TCD can supplement the knowledge gained from CT and MRI scans and can offer crucial information regarding the chances of effective revascularization. TCD can also assist in identifying individuals who might benefit from other therapies like systemic thrombolysis or supportive care but are not candidates for thrombectomy.
Artificial intelligence
With the advent of new imaging methods and algorithms, the use of imaging for patient selection for thrombectomy has improved over time. For instance, artificial intelligence (AI) and improved imaging algorithms can assist in more quickly and correctly identifying eligible patients. AI algorithms are able to examine CT and MRI pictures and provide forecasts regarding the possibility of effective revascularization. These forecasts can aid in directing treatment choices and enhancing the effectiveness of the thrombectomy procedure.
Conclusion
In conclusion, imaging is crucial in determining which patients will have thrombectomy. Important imaging modalities that offer useful information on the location, size, and extent of the blood clot, the underlying cause of stroke, and the viability of brain tissue include CT, MRI, angiography, and TCD. Combining these imaging methods with cutting-edge algorithms like artificial intelligence (AI) can assist find suitable patients and increase the effectiveness of the thrombectomy process.
It is essential for healthcare providers to use these imaging techniques to guide patient selection for thrombectomy and ensure the best possible outcomes for their patients.
Related Articles

Lets get in touch!
Learn more about how Medicai can help you strengthen your practice and improve your patients’ experience. Ready to start your Journey?
Book A Free Demo
