The Modern Radiologist's Guide to Career Growth, Compensation, and Smart Practice
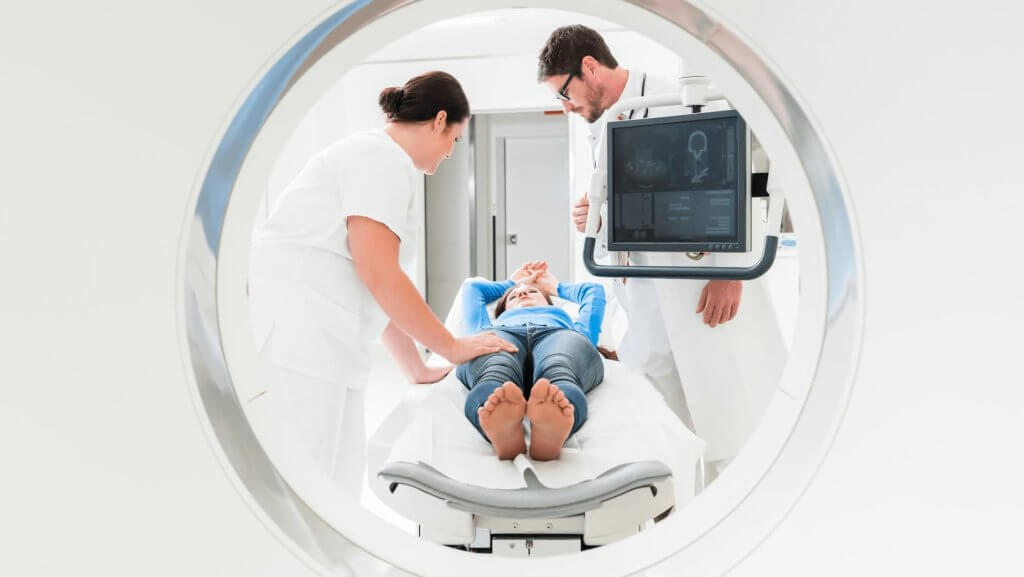
Medicine has never moved faster than it does today. Between AI-assisted reads, shifting reimbursement models, and hospital consolidation, physicians are juggling more change than at any point in recent memory. That makes it harder, and more important, to keep an eye on where your career is actually headed.
Whether you are a resident finishing training or a seasoned attending considering a move, the financial and technological sides of practice deserve more attention than they often get. Salary numbers, workflow tools, and contract terms all add up to the kind of life you build outside the reading room.
Key Takeaways
- Physician pay varies dramatically by specialty, region, and practice setting
- Reliable salary data is one of the strongest tools during contract negotiations
- Imaging technology and AI tools directly affect productivity, and indirectly affect earnings
- Career planning works best when clinical, financial, and lifestyle goals are weighed together
- Transparency benefits both doctors and the institutions that hire them
Why Compensation Conversations Have Changed
For years, doctors were expected to negotiate contracts in the dark. Salary information was guarded, locker-room chats were unreliable, and most physicians had to take an offer at face value or walk away.
That has shifted significantly in the last few years. Younger doctors, in particular, are pushing for more openness about pay, bonus structures, call schedules, and partnership tracks. Hospitals and groups have started responding because top candidates simply expect more.
Being well-informed before a contract conversation does not just help you earn more. It helps you find a role that fits, with realistic expectations from day one. And it reduces the risk of regret a year or two into a job that looked great on paper.
Where to Find Trustworthy Salary Data
National survey data is a starting point, but it rarely tells the full story. Ranges depend on subspecialty, geography, employment model, productivity targets, and even small details like how nights and weekends get covered.
This is where physician-focused resources can make a real difference. Various physician salary data platforms collect compensation data directly from doctors, giving you a clearer picture of what colleagues in similar roles are actually earning. Real numbers from real physicians beat guesswork every time.
When you walk into a negotiation knowing the typical range for your specialty in your region, the conversation becomes more grounded. You can ask better questions, push back where it makes sense, and recognize a fair offer when you see one.

How Practice Setting Influences Earnings
Compensation differs more by practice model than many trainees realize. Private practice, hospital employment, academic medicine, and locum tenens each come with very different financial pictures.
Private practice often offers higher long-term earning potential, especially after partnership, but with more business risk and overhead. Hospital employment usually means a steadier paycheck, predictable hours, and benefits, with less ceiling for growth. Academic positions trade salary for research time, teaching, and stability.
Locum work has surged in popularity for radiologists in particular, partly because remote reading makes the lifestyle more flexible. Day rates can be attractive, although benefits, retirement contributions, and continuity of care look very different than in a traditional role.
Geography and Subspecialty Move the Numbers
Where you practice changes the picture dramatically. Rural and underserved areas often pay more to attract talent, while desirable metro markets tend to come with lower base salaries and a higher cost of living. The best financial deal is rarely in the city you most want to live in, and that tradeoff is one most physicians end up weighing personally.
Subspecialty matters just as much. Within radiology, interventional and neuro work tends to command higher pay than general diagnostic reads, though call burden and procedural volume vary too. The same pattern holds across most fields, where extra fellowship training usually translates into higher earnings over a career.
Group culture is the third lever, and it is the one most candidates underestimate. Two practices in the same city, paying similar base salaries, can feel like completely different jobs once you account for call frequency, vacation, partnership timeline, and how the leadership treats new hires.
The Tech Side of Modern Practice
Technology has quietly reshaped how radiologists earn their living. Cloud-based platforms, mobile-friendly viewers, and AI triage tools are no longer fringe experiments. They are part of how busy departments hit their volumes without burning out staff.
For groups taking on more outpatient or remote contracts, the right imaging platform can be the difference between a smooth workflow and constant friction. Faster sharing, better collaboration with referring clinicians, and clean integration with existing PACS make the practical side of the job easier.
That ease translates into time. And time, in radiology, almost always translates into either more reads or fewer late nights.
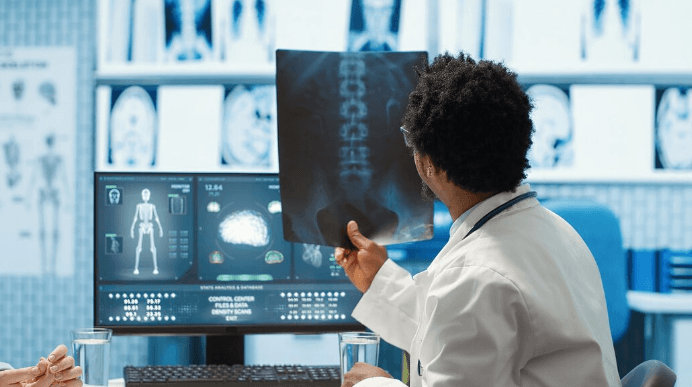
AI Is Not Replacing Radiologists, But It Is Changing the Job
The conversation around AI in radiology has matured. The early panic about replacement has mostly given way to a more practical discussion about augmentation.
Tools that prioritize worklists, flag urgent findings, and pre-measure structures are saving meaningful minutes per case. For a radiologist reading hundreds of studies a week, those minutes add up to better focus on the cases that need the most thought.
Groups that adopt these tools intentionally tend to see productivity gains without sacrificing quality. The radiologists who thrive are the ones who treat AI like a fast junior colleague: helpful, quick, and always worth double-checking.
Building a Career That Lasts
Long careers in medicine are not just about compensation. Burnout, lifestyle, family time, and professional satisfaction all factor in, and they often weigh more heavily as the years pass.
Smart career planning means revisiting your priorities every few years. The role that suited you at thirty-two may not suit you at forty-five, and that is normal. Updating your contract, your tech stack, or even your case mix can keep the work interesting.
Mentorship still matters, too. Honest conversations with colleagues about pay, lifestyle, and the parts of the job they would change are one of the more underused tools in medicine.
Negotiation Tips Worth Remembering
A few practical points come up again and again from doctors who have been through several contract cycles. They are simple, but they make a difference.
First, never accept the first offer without at least asking what is flexible. Bonus structures, vacation, CME funds, and tail coverage are often more negotiable than base salary. Second, get an attorney who reviews physician contracts for a living, not a general practitioner.
Third, do not let politeness keep you from advocating for yourself. Hospitals and groups expect negotiation, and skilled candidates who push respectfully are usually respected for it.
Final Thoughts
Modern medicine asks a lot of physicians, but it also offers more tools and information than ever before. Knowing your worth, choosing the right practice setting, and using technology that actually saves you time can shape both your bank account and your daily experience.
A career in medicine is long. The decisions you make about compensation, tech, and workflow now will compound over decades, so it is worth slowing down occasionally to make sure you are building the practice you actually want.
Frequently Asked Questions
How often should physicians review their compensation? At minimum, once a year, and any time market conditions shift significantly. Reviewing your pay relative to peer benchmarks helps you decide whether to renegotiate, look elsewhere, or stay put with confidence.
Does AI in radiology lower salaries over time? So far, the evidence does not support that worry. AI tools have generally increased throughput and demand for radiologists rather than reducing the need for them, though the role itself continues to evolve.
Is private practice still a good option for new radiologists? For many, yes. Private practice can offer strong long-term earnings and autonomy, but it depends heavily on the group’s structure, volumes, and partnership track. Due diligence matters more here than in employed positions.
What should a fair radiology contract include? At a minimum, clear compensation terms, productivity expectations, call schedules, vacation, CME funding, malpractice coverage including tail, and well-defined termination clauses. A physician contract attorney can flag issues you might miss.How do I know if I am being underpaid? Compare your offer or current pay against multiple sources, including peer-shared platforms, recruiter benchmarks, and conversations with colleagues in similar roles. Persistent gaps across several sources are usually a sign worth acting on.
Related Articles



Lets get in touch!
Learn more about how Medicai can help you strengthen your practice and improve your patients’ experience. Ready to start your Journey?
Book A Free Demo
