Telehealth vs Telemedicine: What Each Term Means, How They Differ, and Why It Matters for Medical Imaging

Telehealth and telemedicine are frequently used interchangeably in healthcare conversations—and are often confused. The distinction matters practically: regulators, payers, and healthcare institutions define the two terms differently, and these definitions determine which services are covered, how they are reimbursed, and what technology infrastructure they require.
The U.S. Department of Health and Human Services defines telehealth as the use of electronic information and telecommunications technologies to support long-distance clinical healthcare, patient- and professional-health-related education, public health, and health administration. The Health Resources and Services Administration (HRSA) describes telemedicine more narrowly as the use of electronic communications and software to provide clinical services to patients without an in-person visit. In the HHS framework, telemedicine is a subset of telehealth — clinical care delivery is one component of the broader telehealth ecosystem.
For a radiology practice, an imaging center, or a hospital radiology department, this distinction has a specific practical implication: the remote interpretation of radiological images — teleradiology — is a telemedicine service in the HHS framework, while the broader infrastructure that enables it — cloud PACS, patient imaging portals, and DICOM sharing platforms — sits within the telehealth ecosystem. Understanding where each element of a remote imaging workflow fits within this taxonomy determines how it is regulated and reimbursed, as well as the technical standards it must meet.
Telehealth vs Telemedicine: How They Differ Across Five Dimensions
The terms telehealth and telemedicine describe overlapping but distinct categories of remote healthcare. The U.S. Department of Health and Human Services and the Health Resources and Services Administration define telehealth as the broader category — covering all remote healthcare services, clinical and non-clinical — and telemedicine as the subset focused specifically on clinical care delivery. The five dimensions below capture the ways in which the two concepts diverge in practice.
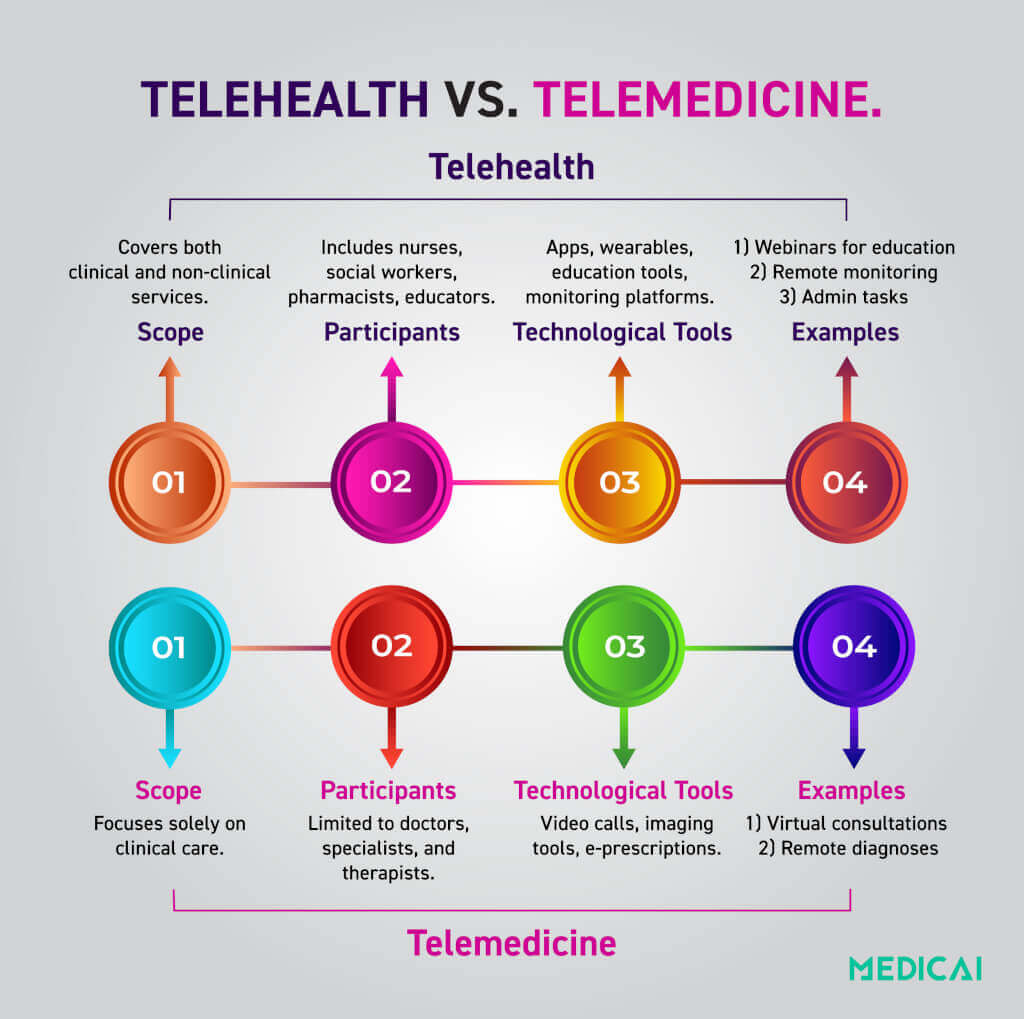
Scope of services. Telehealth encompasses the full spectrum of remote healthcare activity: clinical consultations, provider education and training, administrative coordination, public health monitoring, and patient engagement through health education platforms. Telemedicine is narrower — it covers only the direct clinical interaction between a licensed healthcare provider and a patient for diagnosis, treatment, prescription, or clinical follow-up. A virtual staff training session on updated treatment protocols is telehealth. A video consultation where a physician diagnoses a skin condition and writes a prescription is telemedicine. Both happen on the same platform. Only the second constitutes clinical care delivery.
Technology and infrastructure. Telehealth uses a broad technology stack: mobile health apps, wearable remote monitoring devices, health education platforms, administrative collaboration tools, and the cloud infrastructure — including cloud PACS, patient imaging portals, and DICOM viewers — that stores and serves clinical data to support remote services. Telemedicine uses a subset of that technology stack to enable direct clinical encounters: video conferencing for consultations, secure messaging for clinical communication, digital imaging tools for remote diagnosis, and electronic prescribing systems. In a radiology context, a cloud PACS that archives and serves DICOM studies is a form of telehealth infrastructure. The radiologist using that PACS to interpret a study remotely and produce a signed diagnostic report is performing telemedicine.
Participants. Telehealth involves a wide range of healthcare professionals beyond the physician-patient pair: nurses providing remote patient monitoring, pharmacists offering medication counseling, social workers addressing social determinants of health, educators delivering professional development programs, and administrators coordinating operations. Telemedicine participants are more focused: physicians, specialists, therapists, and psychiatrists delivering direct clinical care to patients. In teleradiology — the telemedicine application most relevant to medical imaging — the participants are the remote radiologist interpreting the study and the ordering physician who receives the diagnostic report.
Clinical applications. Telehealth applications include chronic disease management through continuous monitoring, preventive care education, workforce training and coordination, public health surveillance, and multidisciplinary case discussions. Telemedicine applications are clinical: virtual consultations for acute illness, remote specialist referrals, post-surgical follow-up without in-person visits, telepsychiatry for mental health treatment, and teleradiology for remote image interpretation. The distinction matters practically: CMS reimburses telemedicine services under the Medicare telehealth benefit. Telehealth infrastructure costs — the platform, the monitoring devices, the cloud storage — are generally not separately reimbursable as clinical services.
Regulatory framework. Telehealth regulation covers the technology infrastructure: HIPAA technical safeguards for data storage and transmission, FCC connectivity standards (link: fcc.gov/general/telehealth-telemedicine-and-telecare-whats-what) for broadband access, and state-level technology requirements for remote healthcare platforms. Telemedicine regulation covers the clinical service: state medical licensure requirements (the provider must be licensed in the state where the patient is located), telemedicine-specific practice standards defined by state medical boards, prescribing restrictions for controlled substances via telemedicine, and CMS telehealth billing codes for reimbursement eligibility. The Interstate Medical Licensure Compact streamlines multi-state licensing for telemedicine providers but does not eliminate the requirement to hold a license in each state where patients are seen.
Summary: Five Key Differences Between Telehealth and Telemedicine
| Dimension | Telehealth | Telemedicine |
|---|---|---|
| Scope of services | All remote healthcare services — clinical care, education, training, administration, and public health monitoring | Clinical care delivery only — diagnosis, treatment, prescriptions, specialist consultations, and clinical follow-up |
| Technology and infrastructure | Full stack — mobile apps, wearables, cloud PACS, patient portals, education platforms, administrative tools | Clinical encounter tools — video conferencing, secure messaging, diagnostic imaging viewers, electronic prescribing |
| Participants | Physicians, nurses, pharmacists, social workers, educators, administrators — the full healthcare workforce | Licensed clinical providers and patients — physicians, specialists, therapists, psychiatrists delivering direct care |
| Clinical applications | Chronic disease monitoring, preventive care education, workforce training, public health surveillance, case discussions | Virtual consultations, remote specialist referrals, post-surgical follow-up, telepsychiatry, teleradiology |
| Regulatory framework | HIPAA technical safeguards for infrastructure, FCC connectivity standards, CMS coverage policy for supporting services | State medical licensure in patient’s state, telemedicine practice standards, CMS Medicare telehealth billing codes, ATA clinical guidelines |
Benefits of Telehealth and Telemedicine for Patients And Providers
Let’s see how telehealth and telemedicine have changed medical services for patients and providers.
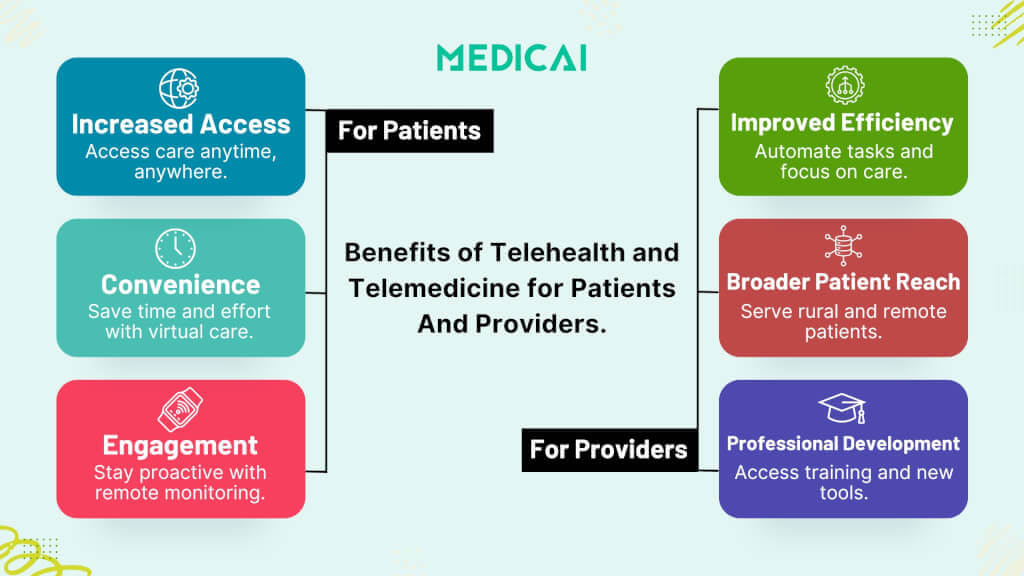
Benefits for Patients
The benefits of telemedicine and telehealth are immense for patient care.
Increased Access to Healthcare Services
It’s not always possible to access healthcare services in rural places. However, telehealth and telemedicine have bridged the gap and brought healthcare to patients’ doorsteps. The beneficiaries include-
- Geographic accessibility, no need to travel a long distance
- Mobility issues like disabilities or chronic conditions
- Specialist availability, such as cardiology or oncology consultation
Convenience
Virtual healthcare indeed saves time and money by optimizing travel. They help with-
- Time-saving – no travel, no sitting in the waiting room, no taking time off work
- Cost-effective – no spending money on fuel, public transport, or lodging for long-distance care
- Comfort as you can be at your home while getting the consultation from the specialists
Enhanced Engagement
A more active role in managing your health as a patient – once it was a dream. However, it is the actual scenario thanks to telehealth with its tools and resources. Platforms like Medicai empower patients by giving them access to their imaging and health records.
Telehealth and telemedicine help with the following:
- Continuous monitoring with wearable devices and mobile apps that track vital signals, activity levels, medication adherence, etc.
- Health education – webinars, tutorials, and interactive tools.
- Better communication with secure messaging
Benefits for Providers
For healthcare professionals, telehealth and telemedicine are the answer to efficiency, growth, and reach. Let’s see how.
Improved Efficiency
Telehealth and telemedicine streamline workflow and reduce administrative burdens. Medicai integrates smoothly with the existing system to enrich both services with automating processes like image retrieval and sharing.
Thus, providers can focus mainly on patient care rather than administrative tasks. Telehealth and telemedicine help with:
- Faster consultation – address minor concerns, review test results, follow-up treatments, etc.
- Streamlined workflows – automate appointment scheduling, billing, record-keeping, etc.
- Reduced No-Shows as patients are less likely to miss virtual appointments.
Broader Patient Reach
With telehealth and telemedicine, the providers can reach diverse patient groups, including-
- Underserved or rural areas.
- Out-of-state patients where regulations allow.
- Patients with mobility issues, transportation challenges, etc.
Increased Professional Development Opportunity:
Telehealth provides tools and resources that help professionals to develop their skills. These resources may involve:
- Webinars and online training – virtual conferences, workshops, certification programs, etc.
- Peer collaboration.
- Access to cutting-edge tools such as AI-driven diagnostic tools or advanced remote monitoring.
Telehealth and Telemedicine in Radiology: What the Distinction Means for Medical Imaging
Radiology is one of the medical specialties where the telehealth versus telemedicine distinction is most practically significant — because remote radiology involves both the clinical service (a radiologist interpreting an image and producing a signed diagnostic report) and the non-clinical infrastructure that makes the clinical service possible (the PACS system that stores the image, the DICOM viewer the radiologist uses, and the HL7 workflow that delivers the report to the referring physician’s EHR).
Teleradiology as telemedicine
The American Telemedicine Association defines teleradiology — the electronic transmission of radiological images from one location to another for interpretation by a remote radiologist — as a telemedicine service. Under the HHS definition, it qualifies as telemedicine because it involves direct clinical service delivery: a licensed physician (the radiologist) produces a diagnostic interpretation (the report) that directly informs patient care decisions. The regulatory requirements that apply to telemedicine — state medical licensure in the patient’s state, HIPAA compliance for patient data, and, in some states, specific telemedicine practice standards — apply to teleradiology in the same way they apply to a remote psychiatric consultation or a virtual primary care visit.
The supporting infrastructure for telehealth
The cloud PACS that stores the DICOM study, the patient imaging portal that allows the patient to access their imaging, and the DICOM viewer that enables a referring physician to view images in the EHR — these are telehealth infrastructure components in the HHS framework. They support the clinical service without themselves constituting clinical care delivery. This distinction matters for reimbursement: CMS reimburses the physician professional component of teleradiology (the interpretation) as a telemedicine service. The infrastructure costs — the PACS subscription and image transmission — are not separately reimbursable as clinical services.
What this means for imaging centers evaluating remote reading infrastructure
An imaging center deploying a cloud PACS for teleradiology is procuring telehealth infrastructure to enable a telemedicine service. The infrastructure must meet HIPAA technical safeguard requirements — AES-256 encryption at rest, TLS in transit, role-based access controls, and a signed Business Associate Agreement. The clinical service delivered through that infrastructure — the remote radiologist’s interpretation — must meet the telemedicine practice standards of the state in which the patient is located. Medicai’s cloud PACS on Microsoft Azure provides the HIPAA-compliant infrastructure layer for the telemedicine service, with a zero-footprint, browser-based DICOM viewer that allows the remote radiologist to read from any location without installing thick-client software — see the teleradiology solution page for the full technical architecture.
Challenges and Considerations with Telehealth And Telemedicine
Telehealth and telemedicine have magically transformed medical services, but also come with challenges.
Regulatory and Licensing Issues Across Different States
In the U.S., healthcare providers must hold licenses in their patients’ state. Also, state policies on telehealth reimbursement, service delivery, and the patient-provider relationship are all over the place, making things complicated for patients and providers.
Efforts like the Interstate Medical Licensure Compact (IMLC) aim to streamline licensing to help physicians practice across multiple states.
The Federal Communications Commission’s 2024 Connected Care Pilot Program report found that telehealth services reduced total healthcare costs by an average of 28% for participating patients (FCC Connected Care Pilot Program).
Ensuring Data Security And Patient Privacy
Data security and patient privacy are challenging in telehealth and telemedicine, which depend primarily on digital platforms. To safeguard information, providers need to invest in strong cybersecurity measures.
Besides, providers must ensure that all platforms comply with HIPAA to protect sensitive data.
Medicai’s platform always prioritizes regulatory compliance. Its HIPAA-compliant infrastructure guarantees secure storage and transmission of patient data.
Addressing Technological Barriers
Adoption and accessibility to technologies are other challenges in telehealth and telemedicine. Not all patients have smartphones, tablets, or computers for virtual consultations.
Additionally, senior citizens or rural patients may struggle to use telehealth platforms or devices. Some places may need more reliable high-speed internet, which is crucial for telemedicine sessions.
Telehealth, Telemedicine, and Telecare: What are the Differences?
Although telehealth, telemedicine, and telecare may sound interchangeable, they differ in focus, scope, and application.
| Aspect | Telehealth | Telemedicine | Telecare |
|---|---|---|---|
| Definition | All remote healthcare services — clinical and non-clinical — delivered via electronic communications (HHS definition) | Remote delivery of clinical care — diagnosis, treatment, and management — by a licensed healthcare provider (HRSA definition) | Remote support for daily living, safety, and independence — typically non-clinical monitoring and assistance |
| Scope | Monitoring, education, training, administrative coordination, and clinical care delivery | Direct patient-provider clinical interactions — diagnosis, treatment plans, prescriptions, specialist consultations | Safety monitoring, fall detection, medication reminders, caregiver coordination |
| Radiology application | Cloud PACS infrastructure, patient imaging portals, DICOM viewers, image sharing platforms — the technology layer enabling remote radiology | Teleradiology — remote interpretation of radiological images by a licensed radiologist producing a signed diagnostic report | Remote patient monitoring for patients with chronic conditions managed through imaging (e.g., cancer treatment response monitoring) |
| Regulatory framework | HIPAA technical safeguards for infrastructure; FCC connectivity standards; CMS coverage policy for supporting services | State medical licensure in patient’s state; HIPAA compliance; CMS Medicare telehealth billing codes; ATA clinical practice guidelines | Varies by jurisdiction; generally governed by home care and assisted living regulations rather than medical practice standards |
| Reimbursement | Infrastructure costs generally not separately reimbursable by CMS as clinical services | CMS reimburses qualifying telemedicine services under Medicare telehealth benefit; state Medicaid coverage varies; commercial payer coverage expanding | Limited CMS reimbursement; primarily funded through care packages, local authority funding, or private pay |
| Examples | Remote patient monitoring, health education platforms, cloud PACS image archiving, patient imaging portals | Virtual doctor consultation, telepsychiatry, teleradiology image interpretation, remote specialist referral | Fall-alert wearables, home vital sign monitors, smart medication dispensers, caregiver alert systems |
Frequently Asked Questions
What is the difference between telehealth and telemedicine?
Telehealth is the broader category — it covers all remote healthcare services delivered through electronic communications, including non-clinical services such as health education, provider training, and administrative coordination. Telemedicine is a subset of telehealth — it refers specifically to the remote delivery of clinical care by a licensed healthcare provider, including diagnosis, treatment, prescriptions, and specialist consultations. The U.S. Department of Health and Human Services and the Health Resources and Services Administration both define telemedicine as a component of the broader telehealth framework. In everyday usage, the two terms are often used interchangeably, but in regulatory and reimbursement contexts — particularly CMS billing — the distinction is significant.
Is teleradiology telehealth or telemedicine?
Teleradiology — the remote interpretation of radiological images by a licensed radiologist — is telemedicine in the HHS regulatory framework, because it involves direct clinical service delivery by a licensed physician that informs patient care decisions. The cloud PACS infrastructure that stores and transmits the DICOM images is telehealth infrastructure — it supports the clinical service without itself constituting clinical care. CMS reimburses the radiologist’s professional interpretation component as a telemedicine service. The PACS subscription and image transmission costs are infrastructure costs not separately reimbursed as clinical services.
Does telemedicine require a PACS system for radiology?
Yes — effective telemedicine for radiology requires a PACS (Picture Archiving and Communication System) that can store, retrieve, and serve DICOM studies to a remote radiologist in a zero-footprint browser-based viewer without thick-client software installation. A cloud PACS on enterprise-grade infrastructure — with HIPAA-compliant AES-256 encryption, a signed Business Associate Agreement, and DICOMweb WADO-RS API for fast study retrieval — is the infrastructure standard for teleradiology as a telemedicine service. On-premise PACS systems require VPN access for remote reading, which introduces latency and security complexity that cloud-native alternatives eliminate.
How does CMS reimburse telehealth and telemedicine services?
CMS reimburses qualifying telemedicine services under the Medicare telehealth benefit, which expanded significantly during and after the COVID-19 public health emergency. Reimbursable telemedicine services include virtual office visits, telehealth mental health services, remote physiologic monitoring, and — relevant to radiology — the professional interpretation component of teleradiology services, billed under the appropriate TC/26 modifier structure. The CMS Medicare telehealth coverage page maintains the current list of covered services and applicable billing codes. State Medicaid coverage for telemedicine varies significantly and should be verified with the relevant state Medicaid program.
Conclusion
Telehealth and telemedicine are transforming healthcare, making it more accessible and patient-focused. While telehealth covers a wide range of remote services, telemedicine focuses on clinical care.
Platforms like Medicai enhance these innovations by offering secure, efficient tools for seamless collaboration, better outcomes, and a connected healthcare future.
Related Articles



Lets get in touch!
Learn more about how Medicai can help you strengthen your practice and improve your patients’ experience. Ready to start your Journey?
Book A Free Demo

