Radiology Revenue Cycle Management: From Imaging Workflow to Reimbursement

Radiology revenue cycle management (RCM) is the end-to-end process by which a radiology practice or imaging center converts a completed imaging study into collected revenue. It begins the moment a physician places an imaging order and ends only when the final balance is posted and collected. Between those two points — through insurance verification, prior authorization, study acquisition, radiologist interpretation, charge capture, claim submission, payer adjudication, and payment posting — every stage has a failure point. And most of those failures do not originate in the billing department. They originate in the imaging workflow itself, before a single claim is submitted.
This guide covers what radiology RCM includes, where revenue is most commonly lost, how the imaging workflow determines billing outcomes, and the performance benchmarks a well-managed radiology practice should meet.
What Radiology Revenue Cycle Management Actually Covers
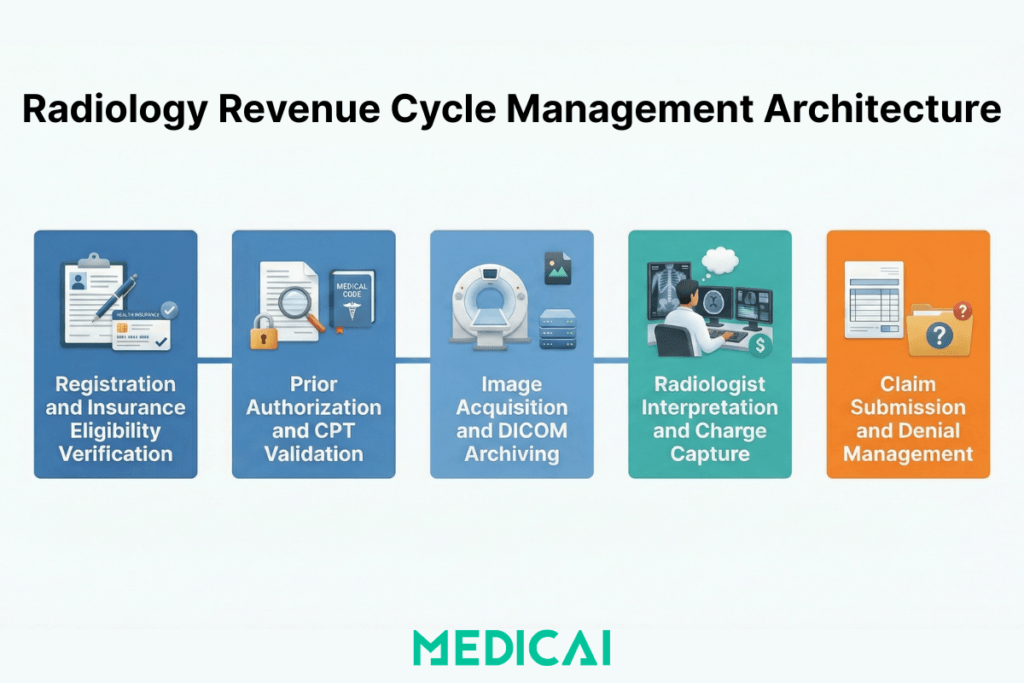
Radiology RCM is broader than billing. The revenue cycle begins at patient scheduling and insurance eligibility verification — before the patient arrives — and ends only when the balance is collected and posted to the practice’s accounts. Between those two points, eight distinct workflow stages each contribute to or subtract from the final reimbursement.
- Patient registration and insurance eligibility verification. Accurate demographics, confirmed active insurance coverage, correct benefit limits, and the right plan type (HMO, PPO, high-deductible) must be captured at the point of scheduling. Errors at this stage — a transposed date of birth, an incorrect group number — result in denials weeks later, after the claim has already been submitted.
- Prior authorization. Most commercial payers require prior authorization for advanced imaging — CT, MRI, PET — before the study is performed. The authorization number must be obtained in advance, tied to the correct CPT code, the performing facility’s NPI, and the ordering physician’s NPI. A study performed without a valid auth, or with an auth obtained for a different laterality or body part than the one actually scanned, results in a denial that cannot be appealed on clinical grounds, regardless of medical necessity.
- maging order and modality worklist. The imaging order generated in the EHR or RIS must transmit correctly to the PACS modality worklist. Patient demographics, the accession number, and the exam description must populate the modality console exactly as they appear in the order. Manual demographic entry at the modality introduces transcription errors, breaking the link between the image and the billing record.
- Study acquisition and DICOM archiving. Images are acquired and automatically uploaded to the PACS archive as DICOM files. The DICOM study must carry the correct accession number — the unique identifier that links the image to the originating order. A mismatch between the PACS study and the RIS order at this stage creates an unbillable study that billing staff must manually reconcile before a claim can be submitted.
- Radiologist interpretation and report generation. The radiologist reviews the study and dictates or templates a structured report that covers the indication, technique, findings, and impression. The report must be signed before charge capture can begin. Late signing — common in high-volume teleradiology environments — creates a backlog of unbilled studies that age toward timely filing deadlines without the billing team being aware.
- Charge capture. CPT codes are assigned from the signed report, modifiers are applied, and RVU values are confirmed. Charge capture is where coding errors concentrate — wrong modifiers, missing laterality codes, and incorrect complexity level assignments are the most common sources of systematic underpayment that practices fail to detect until a revenue audit surfaces them.
- Claim submission and payer adjudication. A clean claim is submitted within the timely filing window. The clearinghouse validates the claim format, the payer adjudicates it against the patient’s benefits and the practice’s contract, and an electronic remittance advice (ERA) is returned with either a payment or a denial explanation.
- Payment posting, denial management, and appeals. ERAs are reconciled against expected contract rates; denials are worked and appealed within payer deadlines; underpayments are identified and disputed; and patient balances are billed. This is the stage most practices associate with RCM — it is also the stage where upstream failures from stages 1 through 7 arrive fully formed and are hardest to reverse.
Radiology Billing and Coding: Where Revenue Is Won or Lost
Radiology billing is the process of translating a completed imaging study and radiologist report into a billable claim. It requires three inputs to be accurate simultaneously: the correct CPT code for the procedure performed, the correct diagnosis code (ICD-10) that establishes medical necessity for the imaging, and the correct modifier that reflects the billing arrangement between the radiologist and the facility. When any one of these three is wrong or missing, the claim is either rejected at the clearinghouse or denied by the payer after adjudication.
Technical component, professional component, and global billing
The technical component (TC modifier) covers the imaging equipment, facility, and technologist. The professional component (26 modifier) covers the radiologist’s interpretation and signed report. Global billing — no modifier — covers both. Which applies depends entirely on the practice’s contractual arrangement with the imaging facility. A hospital-employed radiologist reading studies performed at that hospital bills globally. An independent radiology group providing professional reads for a hospital that they do not operate, and bills only for the professional component. A freestanding imaging center that owns its equipment and employs its radiologists bills globally for studies performed and interpreted on site. Applying the wrong modifier is one of the most common sources of radiology claim denials because the correct modifier is determined by contract, not by clinical circumstance — and the contract terms differ by payer, by facility, and sometimes by modality.
RVU in radiology: how physicians’ work is measured and reimbursed
Relative Value Units (RVUs) are the unit Medicare and most commercial payers use to calculate radiologist reimbursement. Each radiology CPT code carries a work RVU (wRVU) value reflecting the time, skill, and intensity of the interpretation; a practice expense RVU covering overhead costs; and a malpractice RVU. Total RVUs multiplied by the Medicare Conversion Factor — $32.74 in 2024 — produces the Medicare allowed amount for that service. Practices that track wRVUs per radiologist per period can benchmark productivity, model the revenue impact of adding modality capacity, and identify whether interpretation volume trends are tracking ahead or behind revenue targets.
Prior authorization as the upstream denial trigger
Prior authorization must be obtained before the study is performed — not after. The auth number must match the ordered CPT code, the performing facility’s NPI, and the ordering physician’s NPI exactly. For high-volume imaging centers, the most impactful upstream RCM control is automatically verifying that a valid auth number matching the scheduled CPT code appears on the modality worklist before acquisition begins. Studies conducted without this verification result in denials that are not discoverable until after the claim is submitted — at which point the auth window has typically closed and the denial is unrecoverable.
The Five Most Common Radiology Claim Denial Reasons
Radiology denial rates average 10–15% across most practices, compared to a 5–7% benchmark for well-managed specialties. The five denial reasons that account for the majority of radiology-specific write-offs are distinct from general medical billing denials. They originate upstream in the imaging workflow, not in the billing department — which is why they cannot be solved by improving the billing team alone.
- Missing or invalid prior authorization. Auth not obtained before the study, wrong CPT code on the auth, auth expired before the study date, or the ordering physician NPI on the auth does not match the NPI on the claim. This is the single most common source of large-dollar radiology denials because advanced imaging — CT, MRI, PET — carries the highest per-claim reimbursement and the most aggressive prior auth requirements from commercial payers.
- Incorrect or incomplete DICOM metadata. An accession number mismatch between the RIS order and the PACS study prevents the imaging study from being automatically matched to the billing record. A claim submitted for a professional component interpretation without a verifiable accession number — or with an accession number that does not match the archived study — fails adjudication at payers that validate imaging claims against a facility’s PACS submission records.
- Unsigned or late-signed radiology report. A charge cannot be captured for a professional component interpretation without a signed report in the system. In practices where radiologists sign reports 24–48 hours after acquisition — common in teleradiology arrangements and high-volume outpatient settings — unsigned study backlogs accumulate invisibly until they age past the timely filing window. By the time the billing team discovers the unsigned studies, the claim is unfillable.
- Duplicate claim submission. Resubmitting a corrected claim without the correct claim frequency code (7 for replacement, 8 for void), or submitting both a global and a professional component claim for the same study because the billing arrangement changed mid-contract period, generates duplicate denials that require manual resolution at the payer level and cannot be corrected through standard ERA workflows.
- Medical necessity not established. The ICD-10 code on the claim is not listed in the payer’s Local Coverage Determination (LCD) for the ordered CPT code. The ordering physician’s clinical indication — the reason for the study — must map to a covered diagnosis code. If the radiology report does not include the clinical indication from the original order, or if the structured findings do not support the diagnosis code assigned by the billing team, the payer denies the claim on medical necessity grounds. This denial is particularly difficult to reverse because it requires the ordering physician to submit additional documentation that they may no longer have accessible.
How Imaging Workflow Directly Determines RCM Outcomes
Most radiology billing guides treat the imaging workflow and the revenue cycle as separate domains. In practice, they are the same system operating at different time delays. The decisions made at order entry, modality worklist configuration, acquisition, and report generation determine the quality of the data the billing team receives — and no billing software or billing service can retroactively correct data that was never captured correctly upstream.
A PACS that routes studies correctly — matching every incoming DICOM study to its originating RIS order via the accession number — eliminates the most common source of unbillable studies before they reach the billing queue. A structured reporting system that requires the radiologist to complete all mandatory fields before signing — indication, technique, findings, impression — ensures that every billable study has a complete, codeable clinical document attached before charge capture begins.
For organizations evaluating VNA as the enterprise archive layer that ensures imaging data availability and interoperability over time — including what each claimed benefit actually requires to deliver — the vendor neutral archive benefits guide covers the full evaluation framework.
Structured reporting also enables automated charge capture. When the report template is mapped to CPT codes by body part, modality, and complexity level, the system can propose the correct CPT code at sign-off rather than requiring a coder to infer it from free-text dictation. This reduces coding errors, accelerates claim submission, and surfaces upcoding or downcoding patterns that practice administrators can audit on a per-radiologist and per-modality basis.

Medicai’s structured reporting module connects directly to the PACS archive. Every signed report is linked to the corresponding DICOM study by accession number, with a timestamp that documents when the interpretation was completed. For practices using Medicai as their cloud PACS, this creates an auditable chain from order to image to signed report that the billing team can query in real time — identifying unsigned studies before they age, confirming that every acquired study has a billable report attached, and flagging studies where the imaging findings do not support the diagnosis code on the original order.
The connection between PACS and billing systems has traditionally relied on HL7 v2 message feeds — the PACS sends an ORU message when the report is signed, the billing system receives it, and opens a charge. The problem is that HL7 v2 interfaces are point-to-point, vendor-specific, and fail silently: a broken interface means charges stop flowing without alerting anyone in the billing department. Studies are acquired, read, and signed — and never billed — because the feed between the PACS and the billing system stopped working after a software upgrade on either end, and no error message was generated.
FHIR-native imaging platforms address this by surfacing study metadata, report status, and accession numbers via a standard RESTful API that billing systems can query in real time. When the billing system can pull the current report status directly from the PACS rather than waiting for a pushed HL7 message, unsigned study backlogs become visible before they become timely filing problems, and the link between imaging and billing becomes a monitored metric rather than a silent dependency.
Radiology Billing Software vs Outsourced Radiology Billing Services
Radiology practices evaluating their RCM approach face a binary choice: build internal billing capability supported by dedicated software, or outsource to a radiology-specific billing company. The right answer depends on practice study volume, payer mix complexity, available administrative staff, and the practice’s tolerance for billing performance variability.
| Factor | In-house billing with software | Outsourced radiology billing service |
|---|---|---|
| Best fit by volume | 10,000+ studies per year — sufficient volume to justify a full-time in-house billing team with radiology coding expertise | Under 10,000 studies per year — volume too low to carry full-time radiology billing expertise in-house cost-effectively |
| Coding expertise | In-house radiology-trained coders required — general medical billers without subspecialty training produce systematic CPT code and modifier errors in radiology claims | Radiology billing companies employ coders who work exclusively in radiology CPT codes, modifier rules, and payer-specific LCD requirements — no internal training investment required |
| Denial management | Direct access to PACS, clinical documentation, and the radiologist — report amendments and order clarifications can be escalated without routing through a third party, reducing denial resolution time | Payer relationship depth and structured appeal workflows — but ceiling is determined by data quality from the imaging system, which the billing company does not control |
| LCD and coverage monitoring | Internal team monitors payer LCD updates independently — resource-intensive in multi-payer environments and easily missed when billing staff turnover occurs | Billing company monitors LCD updates across all payers as part of service delivery — material advantage for practices with complex payer mixes or high Medicare/Medicaid volume |
| Visibility into billing performance | Full real-time visibility — practice administrator queries the billing system directly for denial rates, AR aging by payer, collection rates, and unsigned study counts at any time | Visibility depends on the billing company’s reporting cadence and transparency — practices should contractually require monthly KPI reporting covering denial rate, days in AR, and net collection rate |
| Cost structure | Fixed cost — salaries, software licensing, and training — regardless of monthly claim volume fluctuations; overhead continues during low-volume periods | Variable cost — typically 4–8% of net collections — scales with study volume without fixed overhead; cost drops automatically in low-volume months |
In both models, the quality of the imaging system’s data determines the ceiling for billing performance. A radiology billing service working from incomplete PACS data — missing accession numbers, unsigned reports, unverified auth statuses — cannot produce clean claim rates above 90% regardless of their billing expertise. The imaging workflow is always upstream of the billing outcome.
Key Performance Indicators for Radiology Revenue Cycle Management
A well-managed radiology revenue cycle is measured by six KPIs that together describe the health of the full cycle from service delivery to cash collection. Tracking all six — not just collections — is necessary because strong collection numbers can mask poor denial management if write-offs are being used to suppress visible AR aging.
- Clean claim rate. The percentage of claims accepted by the clearinghouse on first submission without rejection. Target: above 95%. A score below 90% indicates systemic coding or demographic data quality problems that originate upstream in the workflow, not in the billing department. A clean claim rate below 85% indicates that the PACS-to-billing data feed is unreliable.
- Denial rate. The percentage of submitted claims denied by payers. Radiology benchmark: below 10%. Rates above 15% warrant a root cause analysis by denial reason code — the distribution between auth denials, coding denials, duplicate denials, and clinical necessity denials identifies whether the primary problem is in the scheduling workflow (auth), the imaging workflow (DICOM metadata and report completion), or the billing workflow (coding and modifiers).
- Days in accounts receivable. The average number of days between the service date and the payment. Radiology benchmark: below 35 days. AR above 50 days indicates either a timely filing backlog caused by unsigned reports, a payer mix weighted toward slow-paying commercial plans, or a denial management process that is not working claims within payer response deadlines. AR aging should be segmented by payer to identify which contracts are driving the problem.
- Report turnaround time. The time from image acquisition to a signed radiologist report. This is an imaging workflow KPI, not strictly a billing KPI — but it is the single largest determinant of days in AR for the professional component. A practice with a 48-hour average report turnaround begins every professional component claim two days behind the technical component claim, and accumulates a permanently lagging AR unless the billing system surfaces unsigned study counts in real time.
- wRVU per radiologist. Work RVUs produced per radiologist per period. Subspecialty benchmarks vary — a body imaging radiologist reading outpatient CT and MRI in a high-volume environment should produce 8,000–10,000 wRVUs annually; a neuroradiologist with a complex case mix may be at 7,000–8,000. Tracking wRVU trends against report turnaround time and denial rate reveals whether productivity pressure is creating report quality problems that are generating downstream billing failures — a pattern that aggregate revenue numbers alone will not expose.
- Net collection rate. The percentage of net collectible revenue actually collected after contractual adjustments, write-offs, and patient payments. Target: above 95% of net collectible. Below 90% indicates either aggressive write-off practices masking uncollected balances, systematic underpayment against contract rates that are not being detected, or patient collection gaps in the self-pay and high-deductible segment that are being written off rather than worked.
Frequently Asked Questions: Radiology Revenue Cycle Management
What is radiology revenue cycle management?
Radiology revenue cycle management is the administrative and clinical process by which a radiology practice or imaging center converts completed imaging services into collected revenue. It covers every step from patient scheduling and insurance eligibility verification through imaging acquisition, radiologist interpretation, charge capture, claim submission, payer adjudication, and payment posting. Radiology RCM differs from general medical billing because it must manage both a technical component — facility, equipment, and technologist costs — and a professional component — radiologist interpretation and signed report — each of which may be billed separately to the same or different payers under different contractual arrangements.
What is radiology RCM, and how does it differ from general medical billing?
Radiology RCM operates under a dual-component billing model. The technical component covers imaging equipment, the facility, and the technologist. The professional component covers the radiologist’s interpretation and signed report. General medical billing typically involves a single provider billing a single service to a single payer. Radiology billing must correctly apply TC, 26, or global modifiers to every claim based on the practice’s contractual arrangement with the imaging facility — and that arrangement varies by payer, by facility, and sometimes by modality within the same facility. Radiology billing also carries modality-specific prior authorization requirements that do not exist in most other specialties, adding an upstream workflow burden that directly affects denial rates.
What are the most common reasons radiology claims are denied?
The five most common radiology-specific denial reasons are: missing or invalid prior authorisation where the study was performed without a verified auth number matching the CPT code, facility NPI, and ordering physician NPI; incorrect DICOM metadata causing an accession number mismatch between the PACS study and the RIS billing record; unsigned or late-signed radiology reports that age past timely filing windows before charge capture begins; duplicate claim submission with incorrect claim frequency codes on the corrected claim; and medical necessity not established because the ICD-10 code on the claim does not appear on the payer’s Local Coverage Determination for the ordered procedure.
How does PACS affect radiology billing?
PACS determines billing accuracy in two fundamental ways. First, every DICOM study must be correctly matched to its originating imaging order via the accession number — a mismatch between the PACS study and the RIS order creates an unbillable study that the billing team cannot submit without manual reconciliation. Second, the PACS is the system of record for report status — whether the radiologist has signed the interpretation and when they did. A PACS that surfaces unsigned study backlogs in real time, integrates with structured reporting to ensure every study has a complete signed report before charge capture begins, and connects to billing systems through reliable FHIR APIs rather than fragile point-to-point HL7 v2 interfaces functions as an upstream billing control. A PACS that lacks these properties is a storage system that billing staff works around rather than with.
What is a good denial rate for a radiology practice?
A well-managed radiology practice should maintain a claim denial rate below 10%, with a clean claim rate above 95% on first submission to the clearinghouse. Denial rates of 10–15% are common in practices without dedicated radiology billing expertise or with a high prior-authorization burden in their commercial payer mix. Denial rates above 15% consistently indicate systemic upstream problems — in prior authorization management, PACS-to-billing data feed reliability, or structured report completion rates — that cannot be resolved by the billing team alone without addressing the imaging workflow that produces the data they work from.
What does a radiology billing service do, and when does outsourcing make sense?
A radiology billing service manages claim submission, denial management, payment posting, and payer follow-up on behalf of a radiology practice. They employ coders trained specifically in radiology CPT codes, modifiers, and modifier rules, and monitor payer LCD updates across the practice’s full payer mix. Outsourcing makes sense for practices with fewer than 10,000 studies per year — insufficient volume to justify full-time in-house billing expertise — and for practices with complex multi-payer environments, where keeping pace with LCD and coverage policy changes is itself a full-time task. In both in-house and outsourced models, the billing company or team can only produce clean claims from the data the imaging system provides. Incomplete PACS data, unsigned reports, and unverified auth statuses create denial exposure that no billing service can eliminate after the fact.
Conclusion
Radiology revenue cycle management is a systems problem before it is a billing problem. The practices that sustain denial rates below 10%, days in AR below 35, and net collection rates above 95% are not simply those with the most experienced billing teams. They are practices where the imaging workflow — from order to worklist to acquisition to signed report — produces complete, correctly matched, timely data that the billing team can act on without manual intervention at every step.
Every unsigned report that ages past its timely filing window, every DICOM study that arrives in the billing system without a matching accession number, and every advanced imaging study performed without a verified prior authorization represent revenue failures that began in the imaging workflow. Understanding where those failures originate — and building the workflow controls that prevent them — is the work that determines what the billing department has to bill from. Everything downstream follows from that.
Related Articles



Lets get in touch!
Learn more about how Medicai can help you strengthen your practice and improve your patients’ experience. Ready to start your Journey?
Book A Free Demo

