AI For Oncology Imaging: Early Detection, Better Outcomes
Cancer detection and treatment are undergoing a radical transformation, and AI is at the heart of this evolution. With its ability to analyze complex imaging data, AI is helping oncologists detect cancer earlier, more accurately, and more efficiently than ever before.
AI is revolutionizing oncology imaging by enhancing tumor detection, automating segmentation, and improving scan interpretation. It enables early diagnosis, tracks disease progression, and predicts treatment response. AI-powered PACS and DICOM also enhance accuracy and efficiency in personalized cancer care.
Let’s explore AI’s benefits for oncology imaging and what this means for the future of cancer detection, diagnosis, and treatment planning.

What Is AI for Oncology Imaging?
In cancer imaging, artificial intelligence (AI) refers to computer programs that can learn from medical images, such as CT scans, MRIs, or mammograms. AI helps detect subtle signs of disease, classify tumors, and assist doctors in making decisions.
The AI learning process in Oncology often involves:
- Machine Learning (ML): Algorithms that identify patterns and improve over time with experience.
- Deep Learning (DL): A specialized type of ML that uses layered networks (inspired by the human brain) to automatically extract features from images—sometimes recognizing details beyond human perception.
Core functions of AI in radiology usually involve-
- Detection: AI highlights potential tumors or abnormal growths in images and helps doctors prioritize patients needing urgent follow-up by detecting abnormalities sooner.
- Segmentation: AI rapidly segments tumors in seconds and generates 3D models, aiding clinicians in understanding their shape and interaction with surrounding organs.
- Interpretation: AI can differentiate between benign and malignant lesions and identify possible molecular markers, such as EGFR mutations in lung cancer. Using advanced algorithms, it also tracks tumor responses to treatments over time.
AI is revolutionizing cancer imaging by enabling advanced tumor analysis by 3D tumor tracking, predicting clinical outcomes, and analyzing tumor genetics from scans. It supports clinicians in monitoring disease progression and tailoring personalized oncology care.
Essentially, AI in cancer imaging acts like a supercharged “second pair of eyes,” helping clinicians.
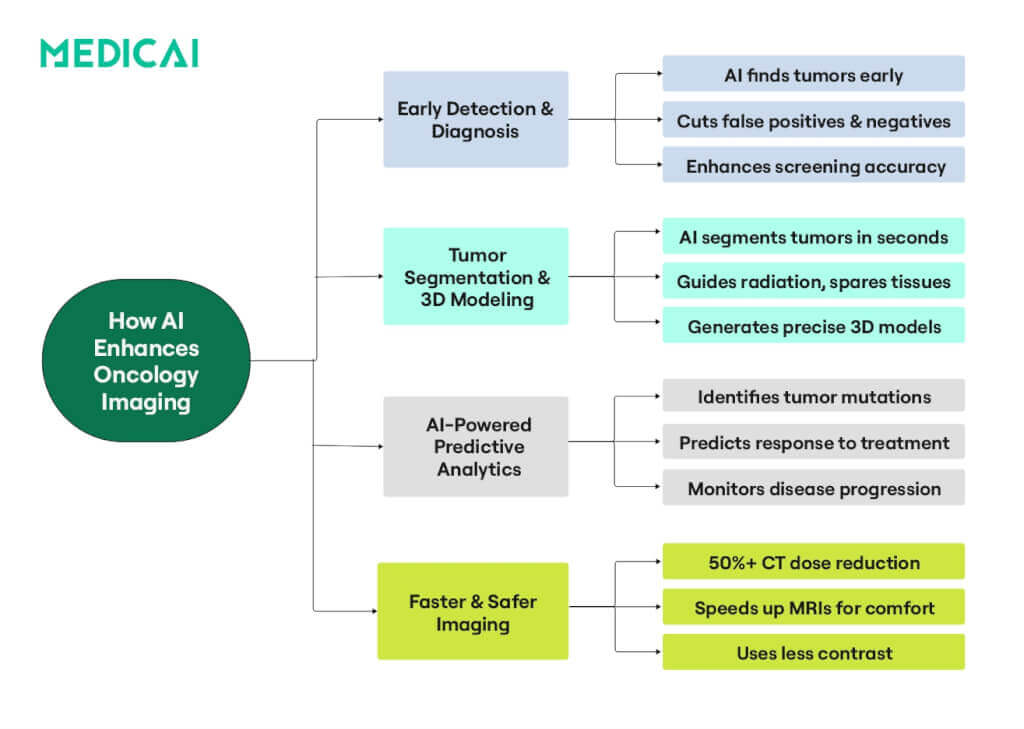
How AI Optimizes Imaging Acquisition and Screening
Cancer patients often undergo frequent imaging, sometimes multiple scans over several years. The cumulative effects of radiation exposure, potential kidney strain from contrast, and the need for reliable, early detection of subtle lesions all demand more efficient and patient-friendly solutions.
AI has emerged as a powerful ally in addressing these challenges and transforming the oncology imaging process.
Reducing Scan Time & Radiation Dose
Deep learning reconstruction (DLR) for computed tomography (CT) enhances image quality using artificial intelligence, potentially providing better patient care. The key advantages include-.
- Less Radiation: AI-based reconstruction uses fewer X-ray projections, markedly reducing radiation. This reduction can significantly lower lifetime risk in pediatric imaging, where tissues are extra sensitive. In fact, deep-learning solutions already demonstrate a 50% or more reduction in radiation dose, preserving diagnostic quality.
- Faster MRI: With fewer raw data points, AI also speeds up MRI scans. This is particularly helpful for patients who struggle to keep still—children, those in pain, or individuals with claustrophobia.
Improving Contrast Efficiency
Gadolinium in MRI can build up over time, and iodinated contrast in CT may strain the kidneys. Lower contrast means fewer side effects; patients often need less prep time before the scan.
Generative adversarial networks (GANs) can reconstruct clear images from much lower contrast doses. Trials report a 50%–90% contrast-dose reduction with minimal accuracy loss.
Lower contrast reduces the risk of contrast-induced nephropathy in patients with renal concerns. Using less contrast also means fewer complications, reduced costs, and smoother post-scan workflows.
Boosting Accuracy in Screening
AI doesn’t tire of maintaining steady accuracy over large volumes of scans. Moreover, AI can provide near-expert screening in remote clinics or places lacking specialist radiologists.
For Lung Cancer (LDCT): Low-dose CT already helps reduce lung cancer deaths. But it can flag many harmless spots. AI refines the process, telling which nodules are malignant and which are likely benign.
AI flags suspicious nodules quickly, helping radiologists prioritize which patients need urgent follow-up.
For Breast Cancer (Mammography & Tomosynthesis): Deep-learning tools excel at spotting early calcifications and minor distortions suggesting malignancy. Besides, AI can lighten radiologists’ load by up to 30% as a second reader, streamlining screening.

AI and In-Depth Tumor Characterization: Beyond Size
Cancer imaging has traditionally focused on measuring tumor size, but AI is changing the game by providing deeper, more precise insights. It ensures that cancer care is more precise, personalized, and ultimately more effective in improving patient outcomes.
Volumetric Segmentation: Precise Tumor Mapping
One of AI’s biggest contributions to cancer imaging is automated volumetric segmentation, which eliminates the need for radiologists to outline tumors slice by slice manually. Instead of working with flat, 2D images, AI constructs a detailed 3D tumor model, capturing the tumor’s true shape, size, and spread.
This mapping enables doctors to monitor tumor changes over time, assessing whether the tumor is growing, shrinking, or responding to treatment. It’s vital for planning radiation therapy, which targets cancer cells while protecting healthy tissue.
AI minimizes human error, enhances the speed and reliability of tumor assessments, and helps doctors make informed decisions.
Radiomics & Imaging Genomics: Decoding Tumor Biology
AI is improving how tumors are measured and revealing what’s happening inside them. A field called radionics allows AI to extract hidden patterns from standard medical scans. It identifies subtle differences in texture, shape, and density that could indicate tumor aggressiveness.
By combining radiomics with imaging genomics, AI can predict a tumor’s genetic makeup from imaging data.
For example, it can identify EGFR mutations in lung cancer, IDH mutations in brain tumors, or MGMT methylation status, which helps doctors determine whether a tumor will respond to specific treatments. This noninvasive approach is particularly valuable when biopsies are difficult or risky.
Intratumoral Heterogeneity: Identifying High-Risk Zones
Not all parts of a tumor are the same. Some areas may be more aggressive, more resistant to treatment, or more likely to spread. This is known as intratumoral heterogeneity, and it’s one of the biggest reasons cancer treatments sometimes fail.
AI can analyze tumor regions to pinpoint areas requiring aggressive treatment versus those responding well to standard therapies. This allows oncologists to adjust real-time treatment plans for more effective, personalized care.
For example, in radiation therapy, AI helps identify tumor areas for higher radiation doses while reducing exposure to healthy tissues, enhancing treatment precision and success rates.
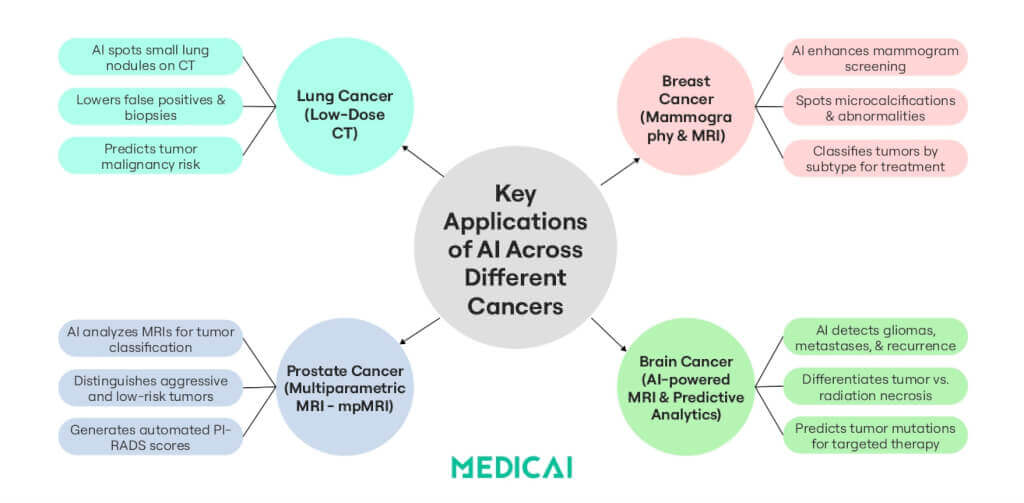
Key Applications of AI Across Different Cancers
Let’s explore some of the key ways AI is transforming cancer management.
Lung Cancer: Enhancing Early Detection and Targeted Therapy
Low-dose CT (LDCT) screening reduces lung cancer mortality by detecting tumors early. However, it can often lead to false positives and unnecessary biopsies. AI enhances accuracy in this process.
- Better Nodule Detection & Risk Scoring: AI models analyze LDCT images to detect lung nodules and identify those at risk of cancer. This reduces false positives and streamlines follow-ups.
- Predicting Tumor Biology: AI can analyze nodules’ shape, density, and texture to predict their growth rate, enabling better treatment planning without immediate invasive procedures.
- Linking Imaging to Genetics: AI can identify EGFR and KRAS mutations—key markers for targeted therapy response. This noninvasive analysis aids doctors in selecting personalized treatments without needing a biopsy.
Brain Tumors: Improving Diagnosis & Treatment Precision
Brain tumors, particularly gliomas and metastases, present diagnostic challenges as imaging can struggle to distinguish between tumor recurrence and treatment-related changes like radiation necrosis. AI is helping with advanced image analysis and predictive modeling.
- Automated Tumor Detection: AI quickly identifies and segments brain tumors, reducing diagnostic uncertainty and aiding in tracking tumor progression.
- Genetic & Molecular Profiling: AI models can predict IDH mutation status in gliomas using MRI scans, aiding in personalized treatment without invasive biopsies.
- Necrosis vs. Relapse Differentiation: AI can analyze subtle imaging features to help determine whether a lesion is an active cancer or a benign post-radiation effect, preventing unnecessary treatments or delays.
Breast Cancer: Enhancing Screening & Personalized Treatment
AI is enhancing mammograms for better breast cancer screening and detection.
- More Accurate Mammogram & Tomosynthesis Analysis: AI models trained on millions of mammograms can detect microcalcifications, masses, and distortions that may indicate cancer.
- MRI-Based Risk Profiling: Breast MRI is often recommended for women at high risk (e.g., those with BRCA mutations). AI enhances MRI interpretation by quantifying breast density and tumor characteristics.
- Improving Cancer Staging & Subtyping: AI can classify breast tumors into ER, PR, and HER2 subtypes, aiding in personalized treatment decisions for hormone therapy and targeted therapies.
Prostate Cancer: Reducing Overtreatment & Unnecessary Biopsies
Prostate cancer is common in men, but not all cases require aggressive treatment. AI helps distinguish between significant and low-risk cancers.
- AI in Multiparametric MRI (mpMRI): Prostate MRI is increasingly used to detect and grade tumors, but interpretation can be subjective. AI models analyze mpMRI scans to provide standardized, objective assessments, reducing variability among radiologists.
- PI-RADS Scoring with AI: The Prostate Imaging Reporting and Data System (PI-RADS) is a grading system used to assess prostate tumors. AI can automatically generate PI-RADS scores, ensuring more reliable, reproducible evaluations of prostate cancer risk.
- Avoiding Unnecessary Biopsies: AI distinguishes between prostate tumors that require biopsies and those that can be monitored, minimizing unnecessary treatments in older patients.
Challenges and Limitations of AI in Oncology Imaging
AI is transforming cancer imaging, but challenges remain in ensuring accuracy, reliability, and ethical use in clinical settings.
Data Quality & Bias
AI models require diverse, high-quality datasets to perform well across different populations. Bias in training data can lead to misdiagnoses and inconsistent performance, particularly in underrepresented groups.
Ensuring multi-institutional datasets and continuous model updates is crucial for fairness and generalizability. To stay updated with evolving AI practices, professionals often rely on tools that turn notes into flashcards for faster learning and retention.
Regulatory & Clinical Validation
For AI to be widely adopted, it must undergo rigorous validation across multiple hospitals and imaging systems. Regulatory approvals (e.g., FDA) are essential, but ongoing monitoring is needed as AI models evolve.
Seamless integration with existing healthcare systems is also a key challenge.
Interpretability & the “Black Box” Problem
One of the biggest concerns in AI-driven oncology imaging is the lack of interpretability—often called the “black box” problem. Many AI models can make accurate predictions, but they often do not explain how they reached their conclusions, such as why a tumor was flagged as malignant.
To address this, researchers are working on:
- Explainable AI (XAI) models that provide visual maps highlighting key imaging features that influenced the AI’s decision
- Confidence scoring to indicate how certain the AI is in its predictions, helping doctors weigh AI recommendations against their clinical expertise
- Human-AI collaboration, where AI acts as a decision-support tool rather than an autonomous system, ensuring that final decisions remain in human hands.
Ethical & Privacy Concerns
AI requires large amounts of sensitive patient data, raising concerns about privacy, security, and consent.
Federated learning helps protect data by training AI across institutions without sharing raw patient information. AI must also be monitored for bias in decision-making to prevent disparities in care.
Conclusion
AI transforms oncology imaging by enabling earlier cancer detection and accurate tumor characterization. It reduces radiation exposure and predicts genetic mutations, improving the efficiency of cancer care.
Medicai integrates AI-enhanced PACS and DICOM systems to provide real-time tumor segmentation and predictive analytics. This helps oncologists make more accurate diagnoses and improve personalized treatment strategies while streamlining workflows and reducing errors.

Related Articles


Lets get in touch!
Learn more about how Medicai can help you strengthen your practice and improve your patients’ experience. Ready to start your Journey?
Book A Free Demo

